How is the breathing rate measured in a person?
Human respiration rate is measured when a person is at rest and involves counting the number of breaths for one minute by counting how many times the chest rises. An optical breath rate sensor can be used for monitoring patients during a magnetic resonance imaging scan. Respiration rates may increase with fever, illness, or other medical conditions. When checking respiration, it is important to also note whether a person has any difficulty breathing. Various other methods to measure respiratory rate are commonly used, including impedance pneumography and capnography which are commonly implemented in patient monitoring.
In addition, novel techniques for automatically monitoring respiratory rate using wearable sensors are in development, such as estimation of the respiratory rate from the electrocardiogram, photoplethysmogram and acceleromatory signals.
What is a normal breathing rate?
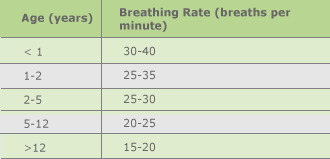
The typical respiratory rate for a healthy adult at rest is 12–20 breaths per minute. Average resting respiratory rates by age are:
- birth to 6 weeks: 30–60 breaths per minute
- 6 months: 25–40 breaths per minute
- 3 years: 20–30 breaths per minute
- 6 years: 18–25 breaths per minute
- 10 years: 17–23 breaths per minute
- Adults: 12-18-breaths per minute
- Elderly ≥ 65 years old: 12-28 breaths per minute.
- Elderly ≥ 80 years old: 10-30 breaths per minute.
What does respiratory minute volume mean?
Respiratory minute volume is the volume of air which is inhaled (inhaled minute volume) or exhaled (exhaled minute volume) from the lungs in one minute.
What does diagnostic value mean?
The value of respiratory rate as an indicator of potential respiratory dysfunction has been investigated but findings suggest it is of limited value. Respiratory rate is widely used to monitor the physiology of acutely-ill hospital patients. It is measured regularly to facilitate identification of changes in physiology along with other vital signs. This practice has been widely adopted as part of early warning systems.
What is considered an abnormal Respiratory rate?
- Apnea
- Dyspnea
- Hyperpnea
- Tachypnea
- Hypopnea
- Bradypnea
- Ortopnea
- Patypnea
- Biot’s respiration
- Cheyne-Stokes respiration
- Kussmaul breathing
What is the science behind stress, heart rate and breathing?
Throughout the day, your heart rate increases or decreases depending on a number of factors – physical demand, chemical interactions (like coffee or nicotine), emotional episodes, and stressful situations. The mechanism by which your heart rate increases in each of these situations is different, as are the implications of the heart rate increase on your overall health and wellbeing. Heart rate control is a balance between the two circuits of the Autonomic Nervous System – the Parasympathetic Nervous System and the Sympathetic Nervous System.
- Sympathetic Nervous System (SNS) referred to as your “fight or flight” system.
- The Parasympathetic Nervous System (PSNS) can be thought of as the “rest and digest” system.
- Together, the PSNS and SNS work in all areas of the body to help you act, react, and recover.
In the heart, although both systems are always running at the same time, the PSNS is the main player in controlling heart rate at rest. Your heart rate starts to increase as the SNS gains more foothold. It is important to note that although SNS activation is normal, certain lifestyle choices we make can cause its activation to be unnatural and prolonged, which can have lasting consequences on our health. The body responds to stress, worry and anxiety in the same ways that it responds to fear and excitement – by activating the “fight or flight” system.
At a chemical level, your body releases a series of hormones that make you hyper-alert, focused, and energized, and this chemical cascade causes increased heart rate, respiratory rate, and perspiration. Consider the archetypal story of the man being chased by the bear. This is the essence of the evolved SNS, or “fight-or-flight” system.
To your body, all these instances are examples of stress, and your body has evolved to prepare you to handle these stressful periods for your survival and to return you to safety. The issue today is that many of us are constantly stressed, worried, or anxious, and as a result, we are overworking our sympathetic nervous system, and not allowing this “return to safety”. One reason the SNS works so beautifully and can come to our rescue when we call is that it usually works in harmony with your “rest and digest” system. You need both, and studies today have shown that when you are under constant stress, your PSNS doesn’t resume control when the battle is done – because the battle is constant – and thus the influence of the PSNS decreases.
Diminished PSNS activity at the mercy of increased SNS activity results in chronic health issues such as anxiety, depression, digestive problems, sleep problems, weight gain, memory impairment, and immune system depression. In terms of the heart, the dire story of stress continues, as the effect of increased heart rate due to stress can lead to high blood pressure, irregular heart rhythms, higher cholesterol, and coronary artery disease.
How can we control this?
Because increased heart rate is an easy indicator of stress, we can combat our stress at a chemical level by recognizing when our heart rate is elevated, and then working to lower it. Fortunately, you hold the power to continuously monitor your heart rate on your wrist (your Basis watch), and you can therefore be an active player in reducing your stress.
How do we lower our heart rate?
One effect of an increased heart rate is increased respiration, or breathing rate. When people are stressed, they tend to take faster, more shallow breaths, in accordance to increased heart rate. This actually differs from faster breathing due to increased heart rate from exercise, and it is this difference that makes breathe control a powerful way to lower your heart rate and stress simultaneously. When you take faster, shallower breaths, are you getting rid of CO2 in the blood faster than normal.
This may seem like a good thing, but in fact, you need CO2 just as much as you need oxygen in your blood, and low levels of CO2 in your blood causes the pH of your blood to change, which can affect the function of your enzymes, organs, and muscles. Low CO2 levels cause psychological effects, such as increased feelings of anxiety and fear, and once these feelings arise, your SNS activates, causing the “fight or flight” cycle to repeat. CO2 is important, and controlling your breath as a way to restore and maintain your CO2 levels in your blood is an important way to reverse the stress cycle, and come back down to homeostasis.
Use your Basis watch to your advantage throughout the day. When you notice your heart rate is increased, take a moment to focus on your breath. Then, try the following exercises to decrease your breathing rate.
- Deep Controlled Breathing; This technique involves deep and slow 10-second inhalation through the nose, followed by a slow and complete exhalation for 10 seconds.
- Diaphragmatic Breathing; The diaphragm is a large, thin dome-shaped muscle that fans out at the base of our lungs. It is our most efficient breathing muscle, but can be compromised in people with chronic stress. In fact, chronically stressed people tend to use their accessory muscles rather than their diaphragm to breathe. This hinders their ability to take deep breaths, which weakens the diaphragm and leads to rapid breaths. By getting more oxygen into your lungs and then into your bloodstream, your muscles will have more fuel and your heart will be able to beat slower and with less effort. In this way, you will interrupt the “fight or flight” response and trigger the body’s normal relaxation, or “rest and digest,” response. When this occurs, the brain will send signals to the various hormone-producing organs, causing smaller amounts of stress hormones to be released. This then enables the liver and kidneys regain control of the stress hormones in the blood stream, and the “fight or flight” response will decrease and ultimately stop.
- Carotid Massage; There are times when you may reach a state of dire stress and anxiety – such as a panic attack. By the time you realize the attack, it seems that you are spiralling downward without rescue. This would be the time to employ the Carotid Massage, which in essence, is a physical way for you to activate the PSNS immediately, and will cause your heart rate, breathing rate, and blood pressure to decrease. The carotid artery runs from your aorta and subclavian arteries, up either side of your neck, and to your brain. You know this artery, because you take your pulse from this artery. In fact, right at the area where you feel for your pulse, there is something called the “carotid baroreceptor”. These baroreceptors have nerve endings that act as sensors so that the brain can detect changes in blood pressure and respond accordingly. The way that the brain responds is by either activating the SNS (if blood pressure is detected as low) or the PSNS (if the blood pressure is detected as high), with the overall goal being to restore normal blood pressure. You can use the carotid massage as a way to “trick” your brain into thinking your blood pressure is high, which will cause it to activate the “rest and digest” response, and lower your heart rate. In order to accomplish the Carotid Massage, take two fingers at your pulse, and gently massage in a circular motion. You should start to feel your body naturally slow down and relax.
What is the normal heart, breathing and blood pressure rates for children?
When the heart or breathing (respiratory) rate is slower or faster than normal, it is often a sign that all is not well. The heart rate (pulse) is elevated when children are unwell. It might just be because they have a fever but it may be something more serious. If the heart rate is slower than normal, particularly in babies, that also can be a sign that not all is well. In babies the easiest place to feel the pulse is on the upper arm above the elbow joint - feel under the biceps muscle. In older children, you can feel the pulse at the wrist.
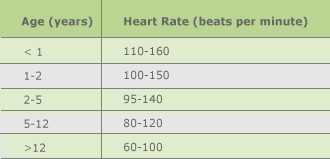
A high respiratory (breathing) rate is usually a sign of breathing difficulty but in children is also seen with heart conditions (like heart failure). Usually when the rate is high due to breathing difficulties, you will also see signs of increased effort or work of breathing.